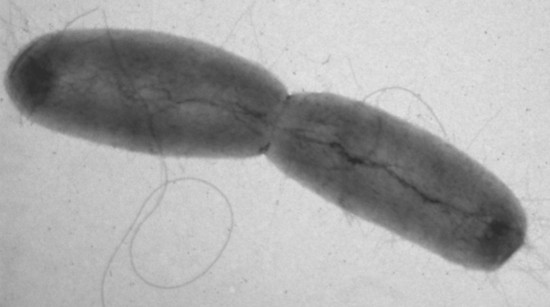
Understanding EHEC Infection: A Growing Concern
The emergence and rapid spread of EHEC (Enterohemorrhagic Escherichia coli) infections in Germany, particularly during a significant outbreak, sent ripples of concern across the nation. This dangerous intestinal bacteria, a specific strain of E. coli, proved to be more formidable than initially anticipated, leading to serious illness and, tragically, multiple fatalities. The initial phase of the outbreak was marked by widespread uncertainty and a desperate search for the source, as public health authorities grappled with an escalating health crisis. Early reports highlighted the devastating impact, with victims ranging from a young woman to two elderly senior citizens over 80, all of whom succumbed to the severe complications induced by these virulent gut pathogens.
The term "Ehec Infektion" quickly became a staple in daily conversations and news reports, underscoring the gravity of the situation. This particular strain of E. coli is known for its ability to produce potent toxins, primarily Shiga toxins, which can cause severe damage to the lining of the intestines and, in some cases, spread to other organs, leading to life-threatening conditions. The initial phase of the outbreak was characterized by a puzzling lack of clarity regarding its origin, fueling public anxiety and emphasizing the critical importance of swift epidemiological investigation in controlling such widespread health threats.
Deciphering the Symptoms: From Mild to Severe
One of the defining characteristics of an
Ehec Infektion is the wide spectrum of symptoms it can present, ranging dramatically in intensity from person to person. While some individuals might experience only mild discomfort or barely noticeable symptoms, others can develop severe, life-threatening conditions. The more severe manifestations typically include intense abdominal cramps, nausea, and critically, bloody diarrhea. This symptom, often referred to as hemorrhagic colitis, is a clear indicator of a serious infection and warrants immediate medical attention.
For a significant portion of those infected, the illness can manifest as acute gastroenteritis, characterized by non-bloody diarrhea that might persist for several days. However, it's the potential progression to more severe forms that makes EHEC particularly dangerous. In a subset of cases, especially in vulnerable populations like young children, the elderly, or those with weakened immune systems, the EHEC toxins can lead to Hemolytic Uremic Syndrome (HUS). HUS is a severe complication characterized by acute kidney failure, hemolytic anemia (destruction of red blood cells), and a low platelet count. This condition is a medical emergency and requires immediate and intensive care.
During the outbreak, observations suggested that women seemed to be disproportionately affected compared to men, where the intestinal bacteria appeared to occur less frequently. While the exact reasons for this demographic difference in susceptibility or reporting were not fully understood at the time, it underscored the need for comprehensive data collection and analysis during public health emergencies. Regardless of demographic factors, recognizing the symptoms of an
Ehec Infektion, particularly the onset of severe nausea and bloody diarrhea, is paramount. If you suspect an EHEC infection, prompt consultation with a medical professional is crucial for diagnosis and appropriate management. Early intervention can significantly improve outcomes and prevent the progression to more severe complications. For more detailed information on initial symptoms and patient experiences, you might find
Ehec Infektion - Article 1 helpful.
The Hunt for the Source: From Mystery to Identification
The early days of the EHEC outbreak were shrouded in mystery, creating widespread uncertainty and, at times, panic across Germany. With the infection spreading rapidly and fatalities mounting, scientists and public health officials were working tirelessly to pinpoint the exact cause. Initial theories ranged from various food sources to environmental contamination, but a definitive link remained elusive. There was considerable speculation that raw, uncooked vegetables might be a potential vector for the bacteria, as some scientists suspected. However, the idea that the contaminated produce might originate from supermarkets was deemed relatively unlikely at the time, primarily because such a widespread source would presumably have led to an even larger number of affected individuals. This period of investigative uncertainty highlighted the immense challenges involved in tracing the origin of foodborne illnesses, especially when supply chains are complex and international.
The media landscape was dominated by daily updates, often featuring the perplexing nature of the EHEC pathogen and its unseen adversary. This lack of a clear source naturally fueled public anxiety, making it difficult for individuals to take targeted preventative measures. As the number of confirmed cases climbed into the hundreds, with at least three initial deaths confirmed, the pressure to identify the source was immense.
The breakthrough finally came with a crucial announcement from Health Senator Cornelia Prüfer-Storcks. The diligent efforts of epidemiologists and food safety experts led to the identification of Spanish cucumbers as the likely culprit responsible for the outbreak. This pivotal discovery allowed for immediate action: the implicated Spanish cucumbers were promptly removed from the market, signaling a turning point in the battle against the spreading infection. The identification of the source was a critical step, offering hope that the rapid spread of the
Ehec Infektion could finally be brought under control. This event underscored the vital role of robust food safety surveillance and rapid response systems in protecting public health.
Preventive Measures and Health Recommendations
The identification of Spanish cucumbers as the likely cause of the EHEC outbreak, while a significant step towards containment, did not negate the ongoing need for caution and robust preventive measures. Public health authorities strongly emphasized that while the immediate source was removed, general principles of food hygiene remain paramount. At the forefront of these recommendations is the thorough washing of fresh produce. Vegetables, especially those consumed raw like salads, cucumbers, and tomatoes, should be meticulously rinsed under running water to remove potential contaminants. Alternatively, cooking or boiling vegetables to appropriate temperatures can effectively kill most harmful bacteria, including EHEC.
Beyond specific actions related to vegetables, broader food safety practices are crucial in preventing the spread of an
Ehec Infektion and other foodborne illnesses. This includes:
- Hand Hygiene: Always wash hands thoroughly with soap and water before handling food, after using the restroom, and after contact with animals.
- Preventing Cross-Contamination: Use separate cutting boards and utensils for raw meat and produce. Ensure raw meat juices do not come into contact with ready-to-eat foods.
- Proper Cooking: Cook meats to safe internal temperatures, as specified by food safety guidelines, to eliminate harmful bacteria.
- Safe Storage: Refrigerate perishable foods promptly and keep refrigerators at appropriate temperatures (below 5°C/41°F) to slow bacterial growth.
Should symptoms such as severe nausea, abdominal pain, or particularly bloody diarrhea become apparent, it is absolutely essential to seek medical attention without delay. Self-treatment can be dangerous, as EHEC infections, if left untreated or improperly managed, can lead to severe complications like HUS. Medical professionals can provide accurate diagnosis, monitor the infection's progression, and offer supportive care, which is critical in managing this potentially life-threatening condition. Understanding and adhering to these guidelines significantly reduces the risk of contracting or spreading an
Ehec Infektion. For additional prevention tips and a deeper dive into safe food handling, consult
Ehec Infektion - Article 2.
Navigating Future Outbreaks: Lessons Learned and Continued Vigilance
The EHEC outbreak served as a stark reminder of the complexities and vulnerabilities within our global food supply chains and the critical importance of public health surveillance. The period of intense uncertainty and the subsequent identification of the source, followed by swift market action, provided invaluable lessons for future public health responses. One of the most significant takeaways was the demonstration of how rapidly a seemingly localized problem can escalate into a nationwide, or even international, health crisis, underscoring the need for robust, internationally coordinated tracking and response systems.
The collaborative efforts between scientists, health authorities, and food safety agencies were instrumental in eventually pinpointing the source and implementing control measures. This event highlighted the necessity of investing in advanced epidemiological techniques and laboratory capabilities to rapidly identify pathogens and trace their origins. Furthermore, it reinforced the ongoing importance of consumer awareness regarding food hygiene, even in an era of stringent food safety regulations. Consumers play a vital role in the final steps of food preparation, making thorough washing and cooking of produce, alongside general kitchen hygiene, an indispensable line of defense against foodborne illnesses.
Moving forward, continuous vigilance remains key. While the particular outbreak centered on an
Ehec Infektion linked to specific produce, the principles learned are applicable to a wide range of food safety challenges. Regulatory bodies continue to refine and strengthen standards for food production, distribution, and labeling, aiming to minimize risks from farm to fork. For individuals, maintaining a proactive approach to food safety—being informed about potential risks and consistently practicing good hygiene—is the most effective way to safeguard health against future outbreaks of foodborne pathogens.
Conclusion
The EHEC outbreak was a challenging period that underscored the serious public health threat posed by virulent foodborne pathogens. From the initial bewildering spread and tragic fatalities to the eventual identification of Spanish cucumbers as the source, the incident highlighted the critical importance of rapid epidemiological investigation, public health communication, and stringent food safety practices. While the immediate crisis was managed, the lessons learned regarding an
Ehec Infektion remain highly relevant. Recognizing the varied symptoms, understanding the serious potential complications like HUS, and adhering to fundamental hygiene principles—such as thoroughly washing and cooking vegetables—are crucial for prevention. Continued vigilance from both consumers and regulatory bodies, coupled with swift responses to potential threats, is essential in safeguarding public health against future foodborne challenges.